Six Leadership Readiness Discussion Questions
Payers are developing care models specific to the level of need. For example, on multiple chronic conditions and complex needs, care for homebound patients, and end-of-life care. Or they may focus on specific conditions such as cardiology, oncology, or neurology. There is not a one-size-fits-all care-management strategy. Payers tend to categorize medical conditions by risk.
Risk Categories
For example, the highest risk would be end-of-life and specialty chronic care conditions, such as cancer. The next high risk is complex poly chronic conditions such as diabetes and depression. A rising risk would be primary care treatable conditions such as COPD or hypertension.
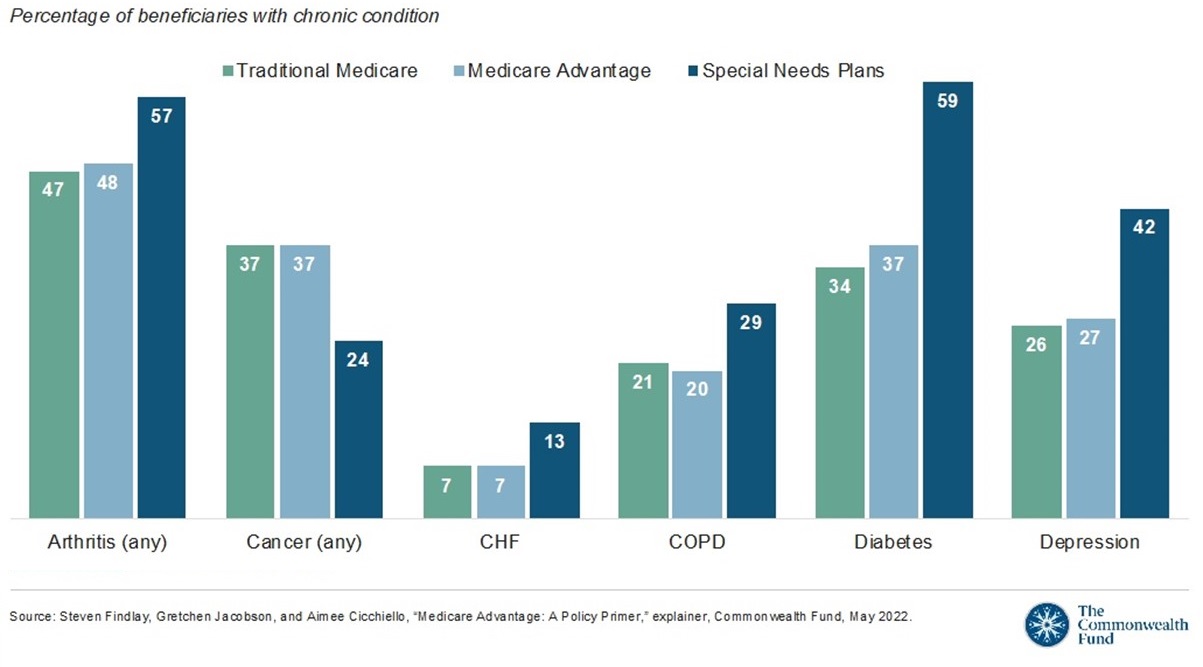
Below is key data for fee-for-service Medicare, Medicare Advantage, and Special Needs Plans, which shows that the prevalence of many chronic conditions is similar for enrollees in traditional Medicare and Medicare Advantage, after separating out Special Needs Plans.
Leadership Readiness Discussion Questions
- How is your organization reducing the cost of care?
- Based on risk, what different technologies are being used?
- What changes based on different medical conditions change the approach for care management and care coordination?
- How is your partnership creating value to manage specific patient populations?
- How can your organization align financial and quality incentives?
- What is the engagement strategy of patients for self-care?

Lisa is a turnaround expert who excels in navigating unsteady, complex, and ambiguous environments. She has provided C-suite education to over 10,000 organizations in the home care sector for decades. Lisa’s trusted voice in the industry has been recognized for her ability to manage disruption, identify new growth and revenue opportunities, and develop high-level engagement strategies between home care and referral partnerships. Her contributions are instrumental in advancing the future of home care.
Other Articles You Might Enjoy
Improving Outcomes Between Home Care and Medicare Advantage Plans
Home care services have emerged as a critical strategy for improving health outcomes, reducing hospital readmissions, addressing both clinical and non-clinical needs, and improved patient satisfaction among Medicare Advantage beneficiaries.
Average 30-Day Readmission Rates by Medical Conditions
We provide critical readmission data about average readmission rates, condition-specific readmission rates, and hospitals with high and low readmission rates.
Hospital-at-Home Readmissions: Which Medical Conditions Created the Highest and Lowest Readmissions?
CMS’s report on the Acute Hospital Care at Home (AHCAH) initiative highlighted the highest and lowest readmission rates by medical conditions.





